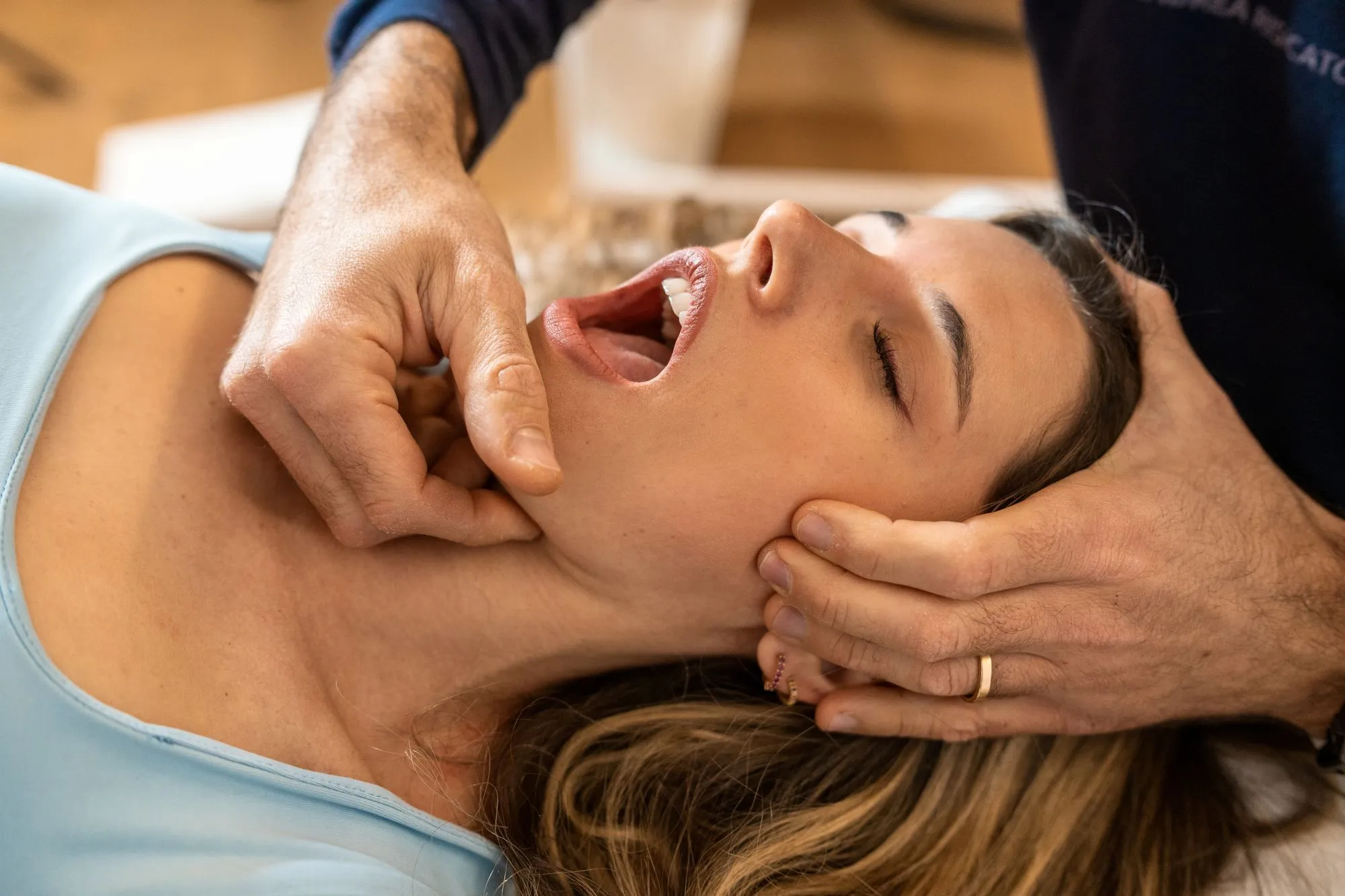
Jaw pain and TMJ dysfunction often require different treatment approaches depending on whether the issue is mechanical, muscular, or neurological. Symptoms such as clicking, limited opening, facial tension, or headaches can present similarly but respond differently to therapy. At Remedial Wellness, treatment selection is based on how the jaw is functioning and how symptoms behave, not just where pain is felt.
Why TMJ Pain Is Often Mismanaged
TMJ pain is frequently treated as isolated muscle tension or generalized stress without identifying the underlying driver. This reflects common clinical patterns rather than all cases, but it often leads to repeated treatments that temporarily reduce discomfort without resolving dysfunction.
A key issue is failing to assess jaw movement. Indicators such as limited opening range, jaw deviation during movement, clicking, or asymmetrical tracking often point to mechanical involvement. When these are not evaluated, treatment tends to focus only on symptom relief.
Another source of mismanagement is not distinguishing between muscle tension and joint dysfunction. Pain that increases with movement or chewing often indicates mechanical restriction, while pain that remains constant regardless of use suggests a sensitivity-driven response. When this distinction is not made, therapy selection becomes inconsistent and recovery is delayed.
How Manual Therapy Addresses Jaw Dysfunction
Manual therapy focuses on restoring movement and reducing mechanical restriction in the jaw and surrounding structures. This includes direct work on the muscles involved in chewing, as well as joint mobilization techniques that improve joint tracking, reduce restriction, and normalize how the jaw opens and closes.
Muscle tension, joint restriction, and movement retraining
Manual therapy is most effective when dysfunction is driven by restricted movement or muscular imbalance. This includes limited jaw opening, clicking associated with movement, or tension that increases with chewing or talking.
Treatment involves reducing muscle tightness, improving joint mobility, and retraining movement patterns. Movement retraining refers to correcting habitual jaw use such as clenching, uneven chewing, or improper opening mechanics that reinforce dysfunction.
Effectiveness is measured through changes in range of motion, reduction in clicking, and symptom improvement within a defined number of sessions. It is less effective when pain is diffuse, constant, or not clearly linked to movement. In these cases, focusing only on mechanical correction may not resolve the underlying sensitivity driving symptoms.
How Acupuncture Treats TMJ-Related Pain
Acupuncture focuses on reducing pain sensitivity and regulating the body’s response to irritation. This refers to lowering perceived pain intensity and altering nervous system response without changing joint structure or mechanics.
Pain signaling, inflammation, and nervous system response
Acupuncture is most effective when symptoms are driven by heightened sensitivity rather than structural restriction. This includes persistent aching, facial tension not tied to movement, or headaches associated with jaw discomfort.
Local irritation around the joint or surrounding muscles can contribute to ongoing pain signaling. Acupuncture targets this response to reduce symptom intensity and improve tolerance.
It is less effective when jaw movement is restricted or when symptoms are clearly triggered by mechanical use. Persistent limitation in opening or deviation during movement indicates a structural issue that requires mechanical correction rather than pain modulation alone.
Situations Where One Therapy Outperforms the Other
Manual therapy tends to outperform acupuncture when jaw movement is restricted, when clicking or deviation occurs during opening, and when symptoms increase with use such as chewing or speaking.
Acupuncture tends to outperform manual therapy when pain is constant, not clearly linked to movement, or associated with generalized facial tension and headaches.
Manual therapy alone may underperform when nervous system sensitivity is the dominant factor, while acupuncture alone may underperform when mechanical restriction is the primary driver. In borderline cases, the starting point should be based on the dominant symptom pattern, with reassessment used to adjust direction.
TMJ pain can be worsened by mismatched treatment. Aggressive manual work on sensitive or inflamed tissue can increase irritation, while relying only on pain modulation without addressing restriction can prolong dysfunction.
Can Manual Therapy and Acupuncture Be Combined?
Combining therapies can be appropriate when both mechanical dysfunction and pain sensitivity are contributing to symptoms. This is most relevant when movement restriction and persistent pain are present at the same time.
Manual therapy addresses joint and muscle function, while acupuncture reduces pain response and muscle guarding. When both factors are present, combining approaches can improve overall response compared to addressing only one.
Combination therapy should follow defined reassessment intervals rather than being applied continuously. It is justified when multiple contributing factors are clearly identified, not as a default approach.
Selecting the Right TMJ Treatment in Edmonton
Selecting the right treatment begins with identifying whether symptoms are driven by movement dysfunction, pain sensitivity, or a combination of both. Jaw pain that changes with movement typically indicates a mechanical issue, while constant pain suggests a sensitivity-driven response.
Patients should begin with the therapy that matches the dominant symptom pattern rather than applying multiple approaches at once. A defined evaluation window should be used to measure progress. If there is no measurable improvement within that period, the treatment approach should be adjusted rather than continued without change.
This structured approach helps avoid over-treatment and reduces ineffective therapy cycles. Clinics like Remedial Wellness apply this method by aligning therapy selection with symptom behavior and using clear checkpoints to guide treatment decisions.